
Patti Lyons, 61, of Doylestown, is the proud owner of Peace Valley Lavender Farm. Five years ago, she received a diagnosis of rectal cancer. Today, she is sharing her story of healing. Patti says the compassionate care she received and the special connection she formed with her colorectal surgeon played an equally important role in her decisions to receive her care at Doylestown Hospital. "You don't appreciate how important it is to have this level of expertise and service close by until you need it," says Patti.
Doylestown Hospital recently earned a three-year accreditation from the National Accreditation Program for Rectal Cancer (NAPRC), a quality program of the American College of Surgeons. Only four hospitals in Pennsylvania hold this prestigious distinction, and ours is the only one in Bucks County.



Lauren Robinson, 36, was in the home stretch of her second pregnancy when she developed severe itching on her palms and the bottoms of her feet.

Fast Action Saved His Leg: Why Primary Care Access Matters More Than Ever
Frustrated at having to wait weeks or months for a primary care appointment, Dennis Rodkey, 56, turned to the web to search for a practice offering timely appointments, quality care, and a provider who accepted his health insurance.

Men’s Health 101
June is Men’s Health Month and a great time to recognize some health challenges men face. According to the Centers for Disease Control (CDC), males in the U.S. can expect to live five years less, on average, than females born in the same year.


Advocating for a Better Patient Care Experience: PFAC

Penn Medicine Doylestown Health Top Docs 2025
Philadelphia Magazine names 84 Penn Medicine Doylestown Health physicians to it’s annual list of Top Docs.
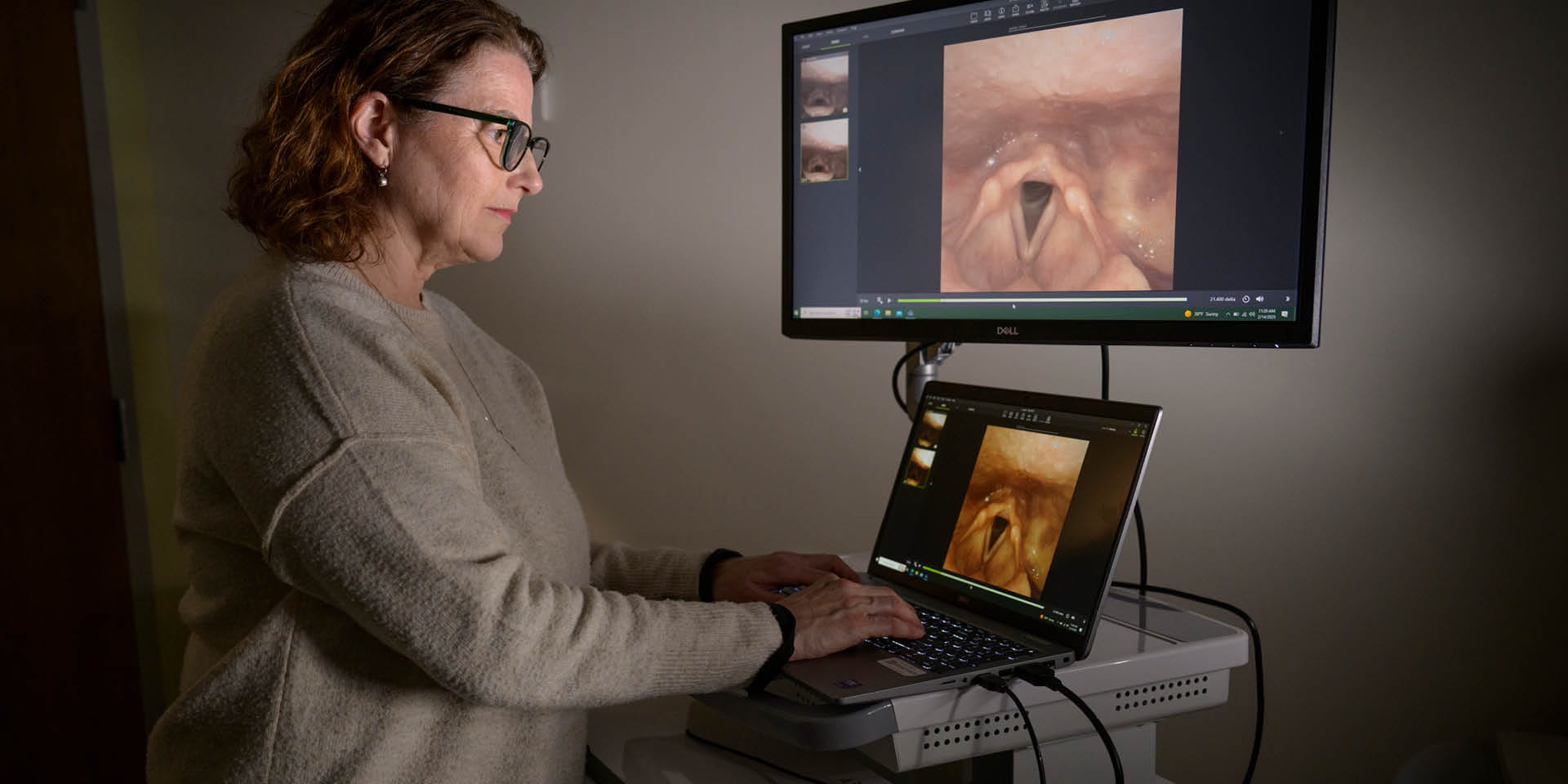
New Tool Enables Precise Swallowing Assessments at the Bedside

Doylestown Health officially joined the University of Pennsylvania Health System, strengthening a shared commitment to delivering the most advanced, convenient and compassionate care to patients and families.