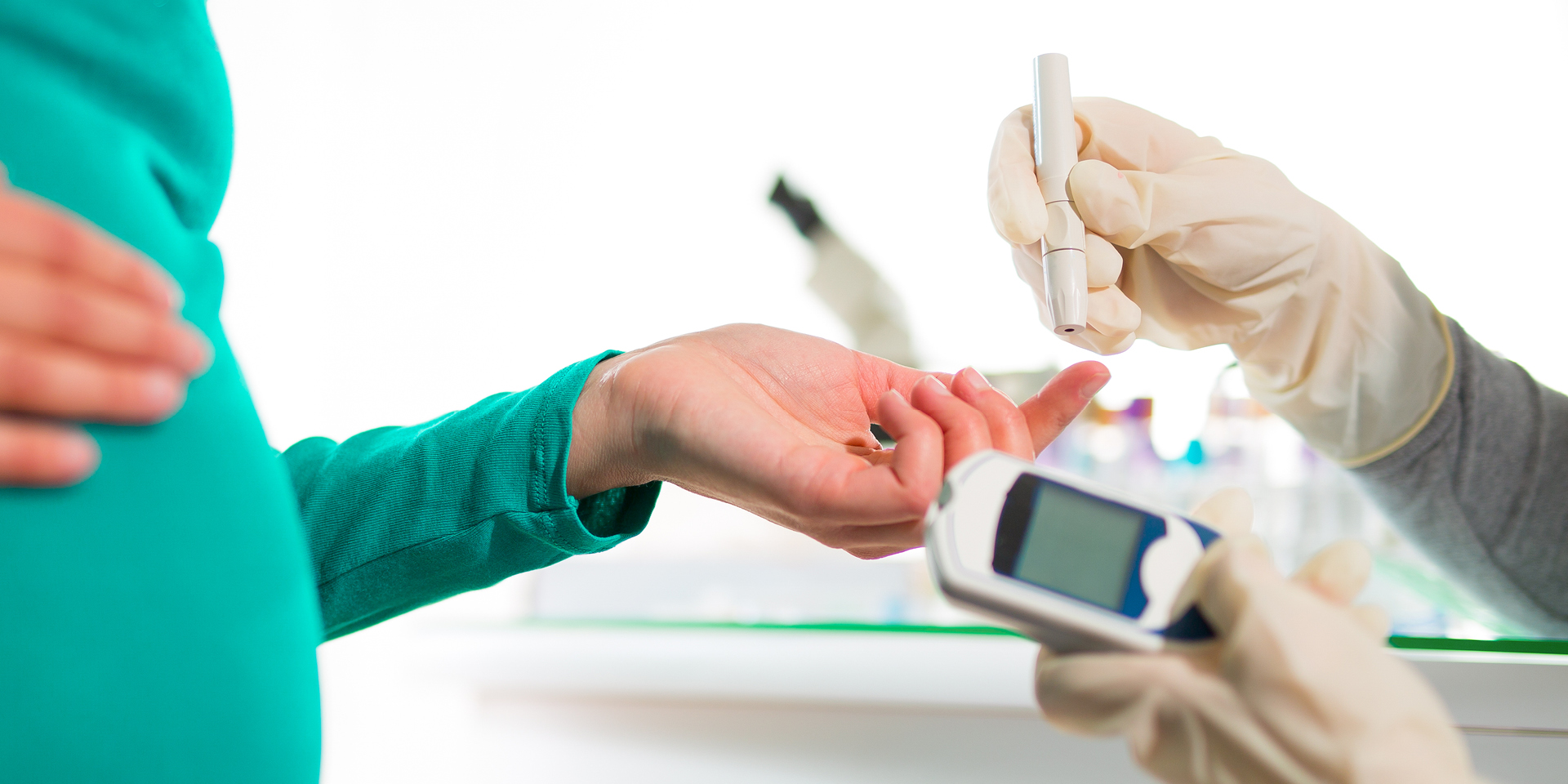
Gestational diabetes can lead to other health conditions; however, women who receive appropriate medical care for gestational diabetes typically deliver healthy babies, according to Doylestown Health certified nurse midwife, JoAnne Ruth, CNM.
What is Gestational Diabetes?
Gestational diabetes occurs when a woman who has not had diabetes in the past develops diabetes during pregnancy, a condition that affects between 2 and 10 percent of pregnancies in the United States, according to the Centers for Disease Control and Prevention (CDC). Diabetes is a disease that occurs when a person's blood glucose, also called blood sugar, is too high.
Pregnancy hormones that support the baby's growth can interfere with the effectiveness of insulin, a hormone that helps the body convert sugar (glucose) into energy. In some cases, this leads to an abnormal buildup of sugar in the blood during pregnancy (gestational diabetes).
Risk Factors
Risk factors for gestational diabetes include:
- Gestational diabetes in past pregnancy
- Family history
- Obesity
- Previous baby weighing 9+ pounds at birth
- Age over 35
- High blood pressure
- Polycystic ovarian syndrome (PCOS), a condition in women who have an increase in male-type hormones (androgens)
Symptoms
- Thirst
- Frequent urination
- Weight gain
- Sometimes, no symptoms
Screening for Gestational Diabetes
"Symptoms of gestational diabetes aren't always clear-cut," explains JoAnne. "In general, gestational diabetes sets in closer to the third trimester when the baby is already fully formed. Diabetes that goes untreated in early pregnancy can cause birth defects. That's why we screen urine for sugar during each prenatal visit."
JoAnne continues, "We also perform a glucose tolerance test around 24 to 28 weeks of pregnancy, or sooner if a patient has risk factors." After an overnight fast, blood glucose levels are checked. Then, the patient is given a beverage (glucola) that is premeasured to contain 50 grams of sugar and blood glucose levels are checked again.
"Test results after the beverage measure the body's effectiveness at turning sugar into energy," explains JoAnne. In her practice as a midwife, she offers the option of a special diet or jelly beans in place of the glucola drink for the screening.
Diagnosing Gestational Diabetes
If screening shows higher than normal sugar levels, a second test is given after an overnight fast, with a glucola drink containing 100 grams of sugar. Blood tests are taken before the drink and again at one, two and three hours after. If two out of four tests are abnormal, the patient is diagnosed with gestational diabetes, according to JoAnne.
Managing Gestational Diabetes
If you develop gestational diabetes, your obstetrician or certified nurse midwife will monitor your baby's growth and support you with a personalized care plan and information to help keep your blood sugar under control. Treatments include:
- Healthy diet
- Monitor your blood sugar
- Healthy lifestyle
- Medication or insulin, if prescribed
Diet
"Diet is key to managing gestational diabetes," says JoAnne. "We talk with patients and provide nutritional information. Some patients visit Doylestown Health's diabetes educator and a nutritionist for added support. Recommendations include avoiding processed sugars and replacing foods like white bread and rice with complex carbohydrates such as whole-grain breads and brown rice. If the patient follows the diet and her sugars are good, she will need a monthly ultrasound to check the baby's growth and we deliver the baby around the due date."
Glucose log
"Patients receive a glucose log, and we go over the entries at every appointment, especially if the patient requires insulin," says JoAnne. "Depending on the patient's needs, she may be given a blood glucose meter to check blood sugar levels throughout the day."
When insulin is needed
If a patient is insulin-dependent, they have more testing including non-stress tests and amniotic fluid checks after around 30 weeks.
When patients require insulin, JoAnne works collaboratively with obstetrician/gynecologist Scott Dinesen, DO, reviewing the patient's case and adjusting insulin as needed.
Effects on Mother
Gestational diabetes resolves after the pregnancy ends. The condition increases the odds of:
- Need for Cesarean section
- Weight gain
- Problems with skin and other organs
- Infection
- High blood pressure/preeclampsia
- Developing type 2 diabetes later in life
Effects on Baby
When there's too much sugar in the blood stream, the baby gets heavier, and if the baby is too big (macrosomia), there can be problems with getting the baby out.
"Many women with gestational diabetes deliver vaginally; however, higher birth weight presents challenges such as the baby's shoulders getting stuck in the birth canal (shoulder dystocia)," says JoAnne.
Your prenatal care provider will monitor you and your baby and discuss your options. Potential complications include:
- Higher birth weights and body fat (9+) pounds
- Low blood glucose after birth
Can Gestational Diabetes be Prevented?
"There's no definitive way to prevent gestational diabetes; however, a visit to your prenatal care practitioner before pregnancy can help get you and your baby off to a good start," says JoAnne.
"It's always good to get in shape before you become pregnant and to stay active," she says. "Seeing women before they become pregnant provides prenatal care providers an opportunity to talk with patients about risk factors and the benefits of prenatal vitamins and a healthy diet."
Doylestown Health Obstetrics and Gynecology
Doylestown Health's expert OB/GYN physicians and certified nurse midwives provide skilled and compassionate health care throughout all stages of a woman's life, from adolescence through menopause and adulthood. And for families welcoming new babies, Doylestown Health's VIA Maternity Center offers labor, delivery and postpartum care in a state-of-the-art, family-centered facility — complete with a Level II Neonatal Intensive Care Unit staffed round-the-clock by CHOP neonatologists.